



Published Mar 24, 2026
11 minute read

Your gastrointestinal tract (the soft tissues from your mouth to your anus) is a part of the body we often take for granted until it’s causing problems. Your gut is a finely tuned ecosystem and it significantly affects your immune system and even your mood. The gut is often referred to as the ‘second brain.’ In this article, we’re covering how to heal your gut naturally.
Often an unhealthy gut goes unnoticed because the symptoms seem completely unrelated such as a skin condition, neurologic symptoms, immune dysfunction, etc., however, sometimes the symptoms are undeniably due to an issue within the GI tract. These symptoms can be quite unpleasant and downright embarrassing. If you have to scope out where the nearest bathroom is when you are outside of your home or you are regularly up at night with indigestion or acid reflux – that is not normal.
Each gastrointestinal tract (GI) is as individual as the owner. But there are a variety of symptoms that may indicate that all is not well in your digestive system.
Do you struggle with:
If some or all of these symptoms seem familiar, you may have an unhealthy GI tract. Some of the possibilities include: Intestinal permeability (‘leaky gut’), yeast overgrowth, SIBO (small intestinal bacterial overgrowth), or gut inflammation. These are fairly common conditions we see in our office, which can be largely blamed on the Western way of life and the Standard American Diet (SAD).

Intestinal permeability is often referred to as ‘leaky gut’. When your digestive tract works correctly, it functions similarly to your skin – it is a place or protection so that everything that comes in contact with it can’t have direct access to our body but at the same time we absorb what we need and excrete what we don’t need. In the case of skin, this would be sweat. In the GI, we digest and break down food and nutrients which are then absorbed through small areas in your intestinal wall known as ‘tight junctions’.
Once these things are absorbed they have direct access into the bloodstream. At the same time, the intestinal lining prevents the passage of harmful substances in the lumen of the GI tract, including toxins, food particles, viruses, parasites, and bacteria. Think of the wall of your digestive tract as a series of tightly guarded entrances – where the ‘army’ (your immune system) is carefully identifying each visitor and determining whether they are friend or foe. Not only can the tight junctions (doors) open when they shouldn’t but the walls (cells) themselves lose integrity.
Similar to a skin condition like leprosy, your GI tract can develop several ‘open’ areas that lead to the inability to perform its functions. We don’t absorb what we want or need and we ‘leak’ out things that should remain in. When the intestinal wall ceases to do what it is meant to do – protect and filter the contents of your digestive tract correctly – you have a leaky gut. When bacteria and other microorganisms, food debris, and toxins enter the system, your ‘army’ recognizes these as ‘foreign invaders’ and an immune system is triggered. Your body goes into ‘battle’ every time you eat.
Chicken or the egg? Intestinal permeability can be the result of certain diseases, infections, pathogenic bacteria in the GI tract, stress, and medications to name a few but intestinal permeability is also a contributor to inflammatory conditions and autoimmune disease.¹

We advise you to consult a certified Functional Medicine Doctor in order to determine if you have a ‘leaky gut’ and we recommend our Fully Functional® process in order to heal. Intestinal permeability is associated with so many chronic health conditions, including autoimmunity, that it is imperative to address your condition and get on track towards optimal health.
We recommend the following actions for everyone:
Realistically you need to avoid eating wheat and gluten-containing foods, period. Not only does gluten contribute to intestinal permeability, but other foods including wheat, cereal, beans, legumes, and more contain lectins, which can contribute to a leaky gut.² Focus on eating leafy vegetables, wild fatty fish, and drinking bone broth.
NSAID medications, such as ibuprofen and aspirin, can be tough on the tummy.³ They suppress your body’s inflammatory response, but part of that response in your gut, prostaglandin, helps protect your intestinal walls from injury. The evidence is clear that NSAIDs contribute to the breakdown of the lining of the GI tract, even ulcers, and associated intestinal permeability.
We advocate exercise as a great way to get endorphins pumping and for greater mental clarity. Excessive exercise (on a hot day or for more than two hours) can lead to damage of the cells in your gut – and greater intestinal permeability. It is not uncommon for distance runners (running for more than ten hours per week) to experience unpleasant gastrointestinal symptoms.⁴
We know that stress leads to the breakdown of the lining of the GI tract. Every patient that gets admitted to the Intensive Care Unit (ICU) of the hospital gets placed on a medication to prevent what are known as ‘stress ulcers.’ As part of our Fully Functional® process, we recommend that our patients begin stress reduction techniques, including breathing exercises, yoga, meditation, prayer, and journaling.
Good ‘bugs’ in the GI tract are critically important when it comes to immune function and intestinal permeability.⁵ A good multistrain probiotic can benefit everyone.
Gastrointestinal inflammation is where the mucosal lining of your gut is inflamed – that is, your immune system has detected a threat and is attacking indiscriminately. Gut dysbiosis, which is an imbalance of microbes in the gut, can be a major contributor. Sometimes your body is at war with itself, and gut inflammation is often where many chronic autoimmune diseases begin.⁶ If not healed swiftly it may develop into any number of autoimmune diseases including Crohn’s disease or ulcerative colitis.
Inflammation can have a marked impact on the rest of your body. Inflammation in the GI tract is not limited to the gut and is associated with inflammatory processes throughout the body and ultimately disease. At the root of almost all disease is inflammation.

You should seek the services of a certified Functional Medical Doctor to advise you on how to heal your gut naturally.
There are several tactics you can use while waiting to see one of our doctors, they are:
Think of your body’s inflammatory response as a mystery you and your doctor have to solve. Your doctor needs data. Keep a food diary logging what you ate and any symptoms you might be feeling – even if you feel ill many hours after you’ve eaten something, this could still be a symptom of inflammation.
If you’re keeping a food diary, we would advise you not to change your diet too drastically before recording your symptoms. However, it is time to stop eating fried food. The oils used in frying food are incredibly inflammatory – and there is little nutritional value. So be kinder to your gut.
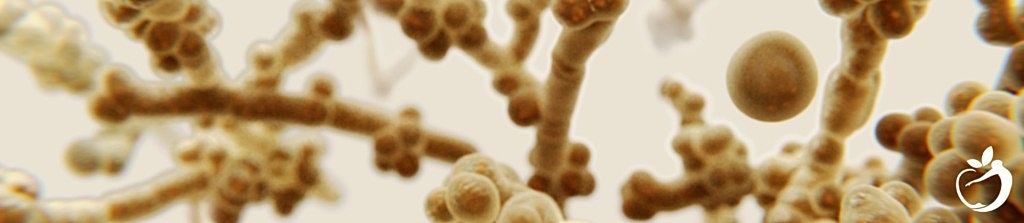
Your gut is home to a trillion microbes and to a form of yeast called Candida albicans. In a healthy gut, the presence of Candida is unremarkable but when it starts to overgrow, you experience discomfort including but not limited to tiredness, headaches, constipation or diarrhea, trapped wind, joint pain, and an increased craving for sweet food.
Before undergoing any drastic changes in your lifestyle, you need to get tested. Consulting a certified Functional Medicine Doctor ensures your body heals holistically as a whole, you’re not seen as just a list of symptoms.
Once Candida overgrowth is detected, we recommend the following lifestyle changes:
Candida feeds on sugar and carbohydrates, so it makes sense that the average American diet fosters yeast overgrowth. You need to cut out refined sugar, bread, pasta, rice, and some dairy. Focus on eating good fats (coconut oil, olive oil, avocados) and plenty of non-starchy vegetables like broccoli, asparagus, and zucchini.
The thought of a cool, crisp beer or glass of wine in the evening may be the only way you get through the day. Unfortunately, most alcoholic beverages also contain carbohydrates – and alcohol itself is inflammatory (see above).
You may feel that you do your best work when you’re stressed, but working or living in a stressful environment affects not only your mental health. Your adrenal glands release cortisol in response to stressful situations, and the more stressed you are, the more cortisol is added to your bloodstream. While cortisol in itself is not a bad thing for your body to produce, it does lower your immune system and increases your chances of yeast overgrowth.
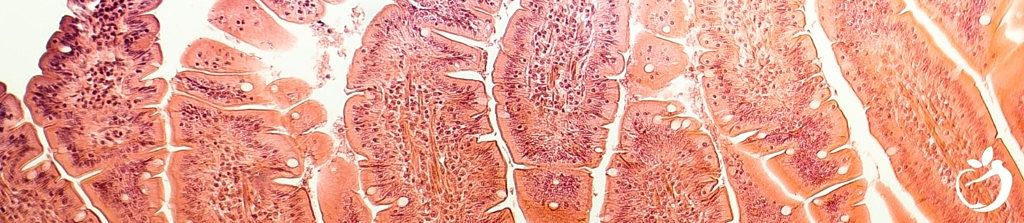
SIBO stands for small intestine bacterial overgrowth, it occurs when there is an overgrowth of bacteria in the small intestine. Your digestive tract is made up of your small intestine and the much larger colon.
Your small intestine usually contains the least amount of bacteria in your digestive system – bacteria is generally found in your colon. As the small intestine is primarily concerned with digesting and absorbing nutrients from food the pH is quite low (acidic) to help achieve this. A low pH is not typically compatible with bacterial growth. Also, the small intestines are tubular in shape, it uses a muscular action to propel the food into the larger colon. This action also usually removes any excess bacteria.
When the normal activity of the small intestine is interrupted or the pH is raised, it leads to a growth of bacteria – and quite often the one-way system between the small intestine and the colon breaks down, and colon bacteria travels up into the small intestine. The bacteria also convert the food they eat into gas and toxins. The gas causes you to experience extreme bloating and wind while the toxins create an inflammatory response, making your symptoms worse.
This bacteria also begins eating the food and nutrients before they can be absorbed into your bloodstream. Your lack of nutrients can often leave you feeling weak, tired, and unable to concentrate. You may lose more weight than is healthy.
There are a number of ways that we can test for SIBO. Once diagnosed, there are several methods for healing your small intestine:
Much of the advice above applies to SIBO. Avoid gluten, dairy, processed sugar, and carbohydrates. Following a low FODMAP diet may be quite helpful. FODMAP is an acronym for the unwieldy term “Fermentable, Oligosaccharides, Disaccharides, Monosaccharides, And Polyols.” FODMAPs are sugars and carbohydrates that are poorly absorbed by the digestive system, leaving them to serve as food for intestinal bacteria. Avoid alcohol and caffeine.
We advise our patients initially to take a course of antibiotics to kill off the bad bacteria. Probiotics are the proactive choice of supplement to take alongside antibiotics if you want to encourage the good, normal bacteria in your gut to flourish.
It’s easy to overlook your digestive concerns – but you must remember that these symptoms are your body’s way of telling you that something is wrong. You must identify the underlying, root cause. If left untreated, leaky gut, inflammation, yeast overgrowth, and SIBO can have serious consequences, often involving an autoimmune disease. When you heal your gut, you’re healing your entire body.
If you are suffering from unresolved gut issues and need a certified Functional Medicine Physician with extensive experience in helping patients overcome their gut issues and live a Fully Functional® life in the Carmel or Indianapolis area, you can book an appointment by clicking here. We are also happy to speak with you at (317) 989-8463, Monday-Thursday, from 8AM – 5PM Eastern time.
Sources: 1 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440529/2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3705319/3 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4266989/4 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1021858/pdf/westjmed00182-0051.pdf5 https://actascientific.com/ASMI/pdf/ASMI-01-0007.pdf6 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1856434/